Medical Jargon Translator & Communication Tool
Translate Clinical Terms
Convert provider labels into patient-friendly descriptionsPractice the "Teach-Back" Method
Use this template to verify your understanding during your next appointment. Copy and adapt this phrase:
"To make sure I've got this right, you're saying that [Clinical Term] means [Your Understanding]. Is that correct?"
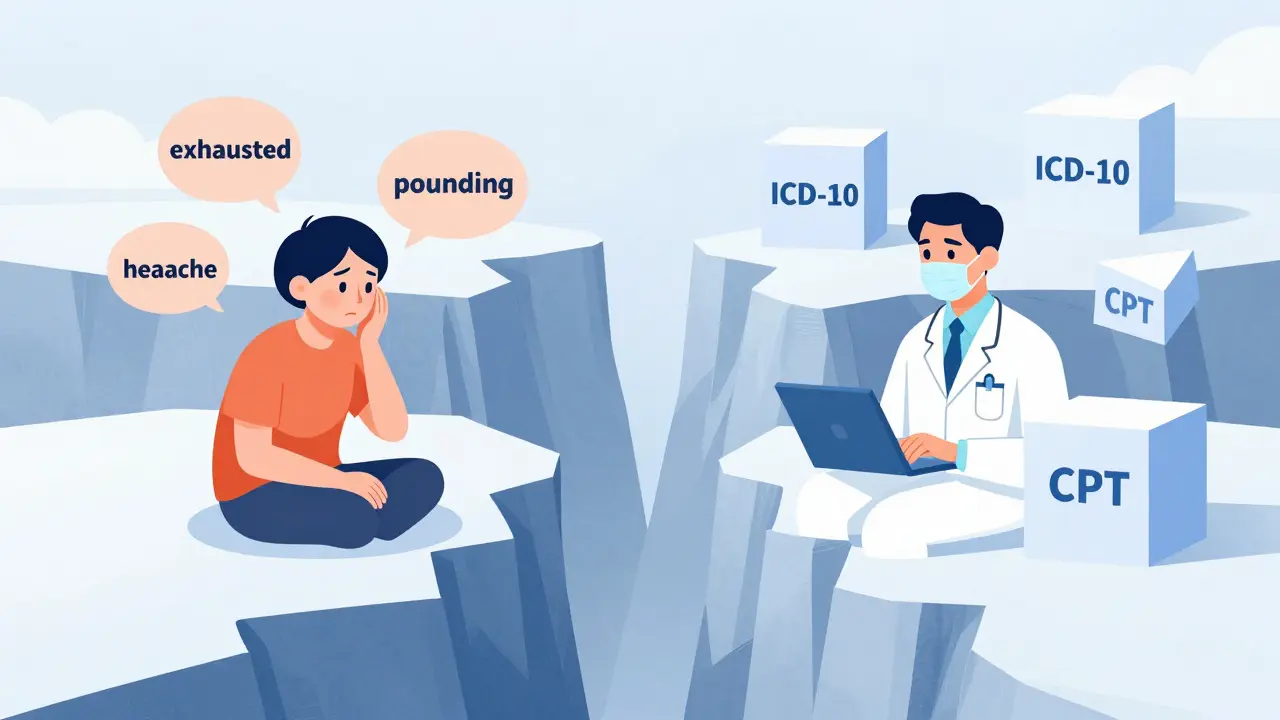
Ever opened your online health portal only to find a phrase like "poorly controlled DM" and wondered if your doctor was judging you as a person? You aren't alone. There is a massive gap between how you describe your health and how a clinic labels it in your chart. While you might talk about feeling "exhausted and thirsty," your provider is typing in ICD-10 is a global standardized system for classifying diseases and health problems codes. This disconnect isn't just a nuance-it's a systemic issue that can lead to serious medical errors and patient anxiety.
The Divide Between Clinical Codes and Human Stories
Healthcare providers operate in a world of precision and billing. To ensure they get paid and to track population health, they use highly structured data. For instance, CPT is a set of medical codes used to describe the services and procedures provided by physicians codes, maintained by the American Medical Association, categorize every single action a doctor takes. These labels feed directly into Electronic Health Records (or EHRs), like the systems used by Epic or Cerner, which prioritize workflow efficiency over conversational clarity.
On the other side, you have "the patient's story." This is experiential and narrative. You don't experience "hypertension"; you experience a pounding headache or a dizzy spell. Research shows this gap is wider than we think. A study in the Journal of General Internal Medicine found that 68% of patients misunderstood common medical terms. For example, 61% of people misidentified the word "colitis," proving that the language of the clinic often feels like a foreign tongue to the people it's meant to help.
How Labeling Differences Affect Your Care
When a provider labels a condition as "metformin 500mg BID," they are being precise. But to a patient, that's just "the white pill I take with meals." When these two worlds don't align, mistakes happen. Dr. Thomas Bodenheimer has noted that this specific language barrier contributes to 30-40% of medication errors. If you don't understand the label on your chart, you're less likely to follow the treatment plan correctly.
The frustration goes both ways. Doctors often spend 15 to 30 minutes per visit just clarifying terms because the labels they use aren't landing. This creates a tension between clinical precision-which is necessary for research and safety-and patient understanding, which is necessary for healing. The 2001 "Crossing the Quality Chasm" report even linked communication failures to 80% of serious medical errors, highlighting that medical labeling differences are a matter of safety, not just semantics.
| Feature | Healthcare Provider Labeling | Patient Information |
|---|---|---|
| Format | Structured, Coded (ICD-10, CPT) | Narrative, Experiential |
| Goal | Billing, Precision, Population Data | Symptom Relief, Understanding, Meaning |
| Example | "Myocardial Infarction" | "Heart Attack" |
| Tool | EHR (Epic, Cerner) | Patient Portals, Memory, Journals |

The Bridge: Health Information Management
So, who fixes this? That's where Health Information Management (or HIM) comes in. HIM professionals are the translators of the medical world. They ensure that the narrative you provide is accurately coded into the clinical labels required for insurance and legal records. They balance the strict requirements of HIPAA is the U.S. law that provides national standards to protect sensitive patient health information from being disclosed without consent with the need for clinical accuracy.
Modern HIM involves more than just filing papers. Specialists undergo hundreds of hours of training in clinical documentation to ensure that a patient's experience is captured without losing the technical detail needed for CMS reimbursement. They are essentially the architects of the bridge between your lived experience and the digital record.

Closing the Gap with New Technology and Laws
We are finally seeing a shift toward "plain language" in medicine. The 21st Century Cures Act was a game-changer, mandating that providers share clinical notes with patients without blocking them. This forced hospitals to realize that if patients are going to read their notes, those notes need to make sense. This has led to the rise of the OpenNotes movement, which has seen a 27% reduction in patient confusion in systems like Kaiser Permanente.
Technology is also stepping in. Some hospitals, like the Mayo Clinic, use templates that automatically swap "myocardial infarction" for "heart attack" when a document is sent to a patient. Even the newer ICD-11, implemented by the WHO, now includes patient-friendly descriptors. We're even seeing AI tools like Google Health's Med-PaLM 2 attempting to translate clinical jargon into human speech, though we aren't quite at the 95% accuracy level needed to let AI handle this without human oversight.
Practical Tips for Navigating the Labeling Gap
You don't have to be a medical coder to get better information from your provider. The best way to bridge this gap is through active communication. The AHRQ recommends a strategy called the "teach-back" method. Instead of just nodding when a doctor explains a diagnosis, try saying: "To make sure I've got this right, you're saying that [X] means [Y]. Is that correct?" This simple flip reduces miscommunication by 45%.
- Ask for plain language: If you see a term in your portal you don't recognize, ask your doctor to "translate" it into a symptom-based description.
- Keep your own log: Record your symptoms in your own words. When you show this to your provider, it helps them map your human experience to their clinical labels more accurately.
- Review your notes: Use your patient portal to check for labels that confuse you before your next appointment so you have a list of questions ready.
Why do doctors use codes like ICD-10 instead of plain English?
Codes provide a universal language that every hospital and insurance company in the world understands. Plain English can be vague; "chest pain" could be anything from indigestion to a heart attack. A specific code ensures the correct treatment is tracked and the provider is reimbursed accurately by insurance.
What is the 21st Century Cures Act?
It is a U.S. law that prevents "information blocking." It requires healthcare providers to give patients easy, digital access to their clinical notes and health information, which is why more of us can now see our doctor's notes in real-time via portals.
Can I ask my doctor to change a label in my medical record?
Yes. While clinical codes (like ICD-10) are based on diagnostic standards, you can request corrections to the narrative parts of your record if you feel the description of your symptoms or history is inaccurate.
How does the "teach-back" method work?
The teach-back method is when a patient explains the provider's instructions back to them in their own words. This confirms the patient understands the information and allows the provider to correct any misunderstandings immediately.
What is the difference between an EHR and a patient portal?
The EHR (Electronic Health Record) is the full clinical database used by providers for charting, billing, and coordination. The patient portal is a "window" into that record, showing a filtered version of the data specifically for the patient to see.

Carol Yang
April 23, 2026 AT 16:59This is actually a really good point. I always felt like I was reading a different language when I checked my portal lol.
Daniel Runion
April 23, 2026 AT 18:55Oh please!!! As if the 21st Century Cures Act is some magical fix for a broken system!!!! It's just more digital noise to make us think we're in control while the EHRs still hoard the real data!!!! Absolute joke!!!!
Ben Jima
April 23, 2026 AT 21:10The teach-back method is a gold standard for a reason. If you're struggling with your provider, try it out. It shifts the responsibility of clarity onto the communication process rather than the patient's intelligence. It's a small change that makes a massive difference in health outcomes.
Brittney Prince
April 25, 2026 AT 03:00Anyone else think these 'patient portals' are just a way for insurance companies to track how often we're actually complaining about symptoms? They want us reading these coded notes so we get confused and just stop asking for expensive tests. It's all a game to keep the money in their pockets and the patients in the dark. Just look at how 'efficient' the EHRs are-they aren't for the patients, they're for the audit trail.
Nila Sawyer
April 27, 2026 AT 02:45I absolutely love the idea of bridging this gap because it brings so much hope for people who feel lost in the medical system! 🌟 It is just so wonderful to think that we are moving towards a world where patients are treated as partners in their own healing journey and not just as a set of ICD-10 codes in a database 💖 I truly believe that with more empathy and these amazing new AI tools, we can make healthcare feel human again for everyone regardless of where they come from or what language they speak! ✨😊
Nikita Shabanov
April 28, 2026 AT 15:27From a technical perspective, the transition to ICD-11 is a significant step. It attempts to integrate traditional medicine and more descriptive categories which should, in theory, reduce the friction between the provider's code and the patient's lived experience. However, the implementation phase is always where the real challenge lies, as updating legacy EHR systems is a monumental task.
Jaclyn Vo
April 29, 2026 AT 20:23Ugh, please!! 🙄 Like I'm actually going to spend my free time 'logging' my symptoms in a diary like it's the 1800s just so my doctor can map it to a code? Give me a break!! If the system is this bad, they can fix it without me doing the work for them! 💅
Sharyl Foster
May 1, 2026 AT 03:13Actually, the 'plain language' movement is mostly surface-level. They swap a word here and there but the underlying logic is still purely for billing. You can call it a 'heart attack' all you want, but if the code is wrong, the insurance claim gets denied and the patient gets the bill anyway. That's the real gap.
James Harrison
May 1, 2026 AT 08:38It's interesting to think about how language shapes our reality. When a person is reduced to a code, the human element of suffering is stripped away to make it manageable for a system. We're basically treating the map as the territory.
William Zhigaylo
May 1, 2026 AT 12:55The sheer incompetence of a system that allows a 30-40% medication error rate due to linguistic failures is utterly abhorrent. It is a systemic failure of the highest order, and the fact that we are only now discussing 'plain language' is an indictment of the entire medical establishment. One must wonder how many preventable deaths have occurred because a clinician could not be bothered to speak plainly.
Vijay AGarwal
May 2, 2026 AT 17:47This is a tragedy of epic proportions! How can we trust our lives to a system where a single mistyped code can lead to a catastrophic error?! It's absolutely wild that we're relying on 'translators' like HIM professionals to keep us from falling through the cracks of a digital abyss! The horror of not knowing what's in your own chart is enough to give anyone a panic attack!
suresh kumar
May 4, 2026 AT 13:05Which portals are you guys using? I bet some of them are way more glitchy than others. My cousin's doctor uses this old prehistoric system that looks like it's from 1995 and it's a total circus. Do you think the AI will eventually just tell us we're dying in plain English or will it keep the fancy codes to save the drama for the end?
Elle Torres Sanz
May 6, 2026 AT 00:42It's so important to remember that for non-native English speakers, this gap is even wider. Imagine fighting through medical jargon in a second language while you're already feeling vulnerable. We need to make sure the 'plain language' shift includes multilingual accessibility and cultural humility so no one is left behind in the digital transition.
sachin singh
May 6, 2026 AT 05:03The mention of the OpenNotes movement is quite promising. If patients can identify errors in their records in real-time, it creates a double-check system that naturally improves data quality. I would be very interested to see more data on how this specifically impacts chronic disease management where long-term tracking is essential.